Healthcare Facilities and MEP Planning

In recent years, Japan has never experienced an outbreak of virus that required countermeasure with infectious diseases so widely as the overwhelming novel coronavirus. However, looking at the world, large-scale measures against spread of viruses such as SARS in Southeast Asia in 2003 and MERS in the Middle East in 2012 have been occurred in around ten years’ time.
In response to the need for continuous countermeasures against such infectious diseases, Nihon Sekkei will introduce some of the environmental and hygienic MEP planning initiatives that have been implemented to date. These accumulated planning method can develop and adapt to healthcare facility projects or other different building types.
It is important to consider effective countermeasures according to the route of infection, in order to design healthcare facilities that take into consideration the infection prevention.
The following (*1) are possible routes of infection:
1.Physical Contact Infection -An infected person holds his or her hand up against their mouth when sneezing or coughing, then touches things around them with that hand, and the virus transfers onto those objects. When a non-infected person touches the objects, the virus is then attached to their hands. And if the person they touches his/her their mouth or nose with the hands, the person will be infected by the virus transmitted through the mucous membranes.
2.Droplet Infection -Infection occurs when large particles (droplets larger than 5 μm) containing viral pathogens come into contact with the mucous membrane or conjunctiva of the nose or mouth of another person.
3.Airborne Infection -Refers to a route of infection through the spread and inhalation of small particles (droplet nuclei less than 5 μm in size) containing viral pathogens. Since droplet nuclei are spread in the ai, special ventilation (e.g. negative pressure chamber) or filters are required to remove them.
4.Others ― Transdermal infections, mother-to-child infections, blood infections (cross infections), etc.
※Some theories advocate aerosol infection as an intermediate form of infection between droplet and airborne infection.
The novel coronavirus is said to be spread by “contact,” and “droplet” among three types of infection routes, “contact,” “droplet,” and “air,” and is isolated from respiratory tract secretions and feces. *1
It is considered that no airborne infection has occurred, but the risk of infection allegedly increases with a large number of conversations in closed space or in short distances * 3 *4. The Ministry of Health, Labour and Welfare therefore has also proposed a ventilation method to improve one of the factors, “closed space with poor ventilation” *5.
Furthermore, Japanese Society for Infection Prevention and Control suggests a room isolation method for hospitals for infected or suspected patients such as “A general patients room with appropriate ventilation method, when it is difficult to provide a negative pressure room,” and “It is suggested to ventilate at least 6 times per hour or more “*2. This indicates the importance of ventilation equipment.
Practice through healthcare facilities
1.Selection and Product Development of Sanitary Equipment as a Countermeasure Against Contact Infection
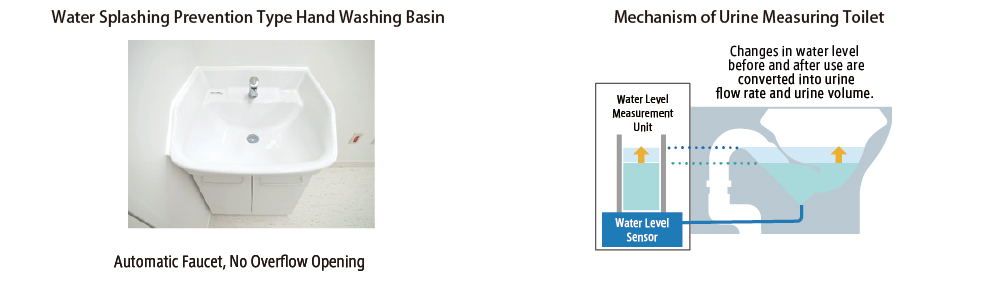
Nihon Sekkei will select handwashing basins for healthcare professionals based on the ease of hygienic maintenance, such as with a raised bowl rim to reduce water splashing to the surrounding area, an automatic faucet that does not come into contact with hands, and a fixture without an overflow opening to prevent bacteria proliferation. Nihon Sekkei is also participating in the product development of urine measuring toilets as a support equipment for urine storage fixtures and automatic urimeters, and save time collecting urine from patients while reducing direct contact.
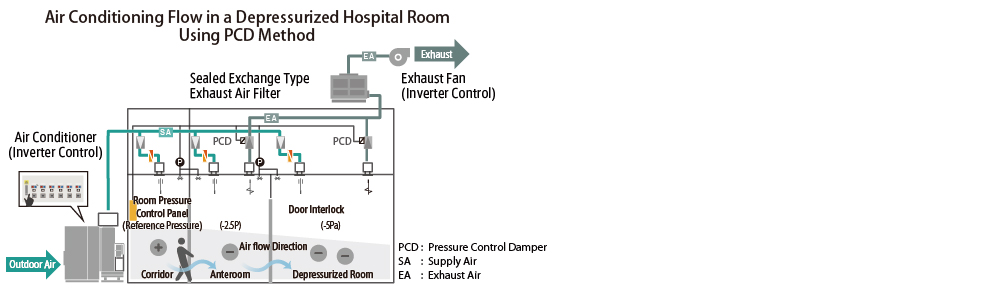
2.Air Conditioning System Plan for Pressure Control in the Hospital Room
In class 1 infectious disease rooms , it is required to be depressurized on as the countermeasure of airborne infection. General hospitals may also be required to have rooms that can be switched between negative and equal pressures, depending on the situation. The PCD (Pressure Control Damper) method, which controls air conditioners, exhaust fans, etc., to maintain the appropriate pressure while measuring the pressure between each room, is a planned system that can achieve depressurized rooms.
Next project introduces a renovation plan that converted to a 500 beds patient ward with a PCD system by remodeling as the variable pressure entire ward department for accommodating patients with infectious diseases in the event of a pandemic.
During normal times, the hospital rooms and corridors are operated at equal pressure, but during a pandemic, the air conditioning control can be switched to depressurize the rooms and keep the entire ward at negative pressure from other areas. Exhaust air is released after filtration through a HEPA (High Efficiency Particulate Air) filter. The air change rate (exhaust volume) of the hospital rooms is set to be at least 6 times per hour.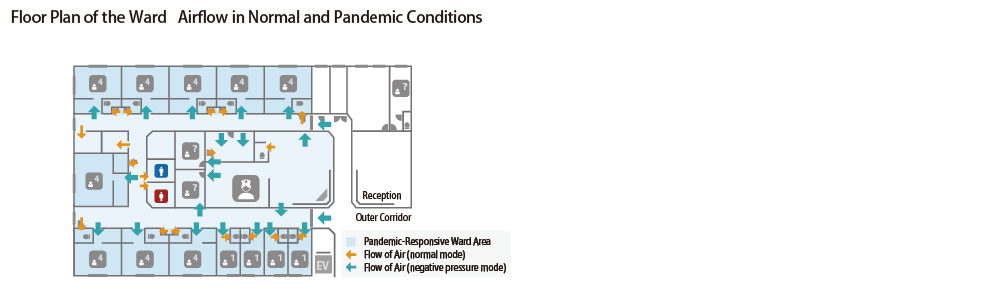
3.Development Examples of Cleaning System to Improve Air Quality
The removal rate of viruses in the air conditioning system by UVGI and TMiP cleaning system in the AC chamber and actively improves the air quality in the room. Joint development with manufacturers and verification tests with universities verify the effectiveness of the technology.
① UVGI (Ultraviolet Germicidal Irradiation) is a system that utilizes UV sterilization lamps for air conditioning, and it has been widely used in the United States. The guidelines of the CDC (Centers for Disease Control and Prevention)*4 in the United States also recommend the use of UV sterilization in healthcare facilities.
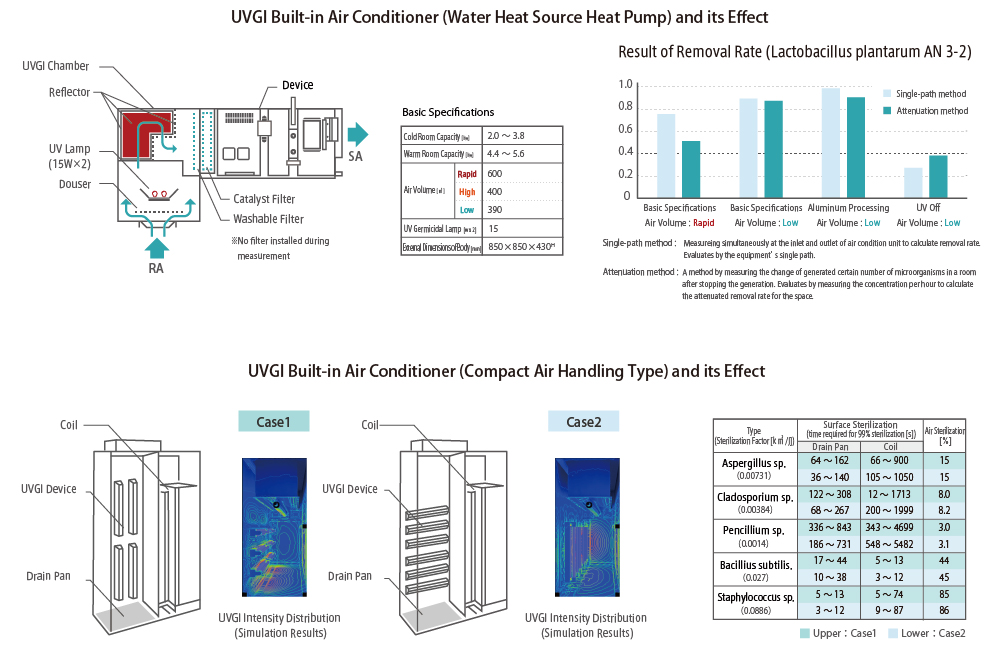
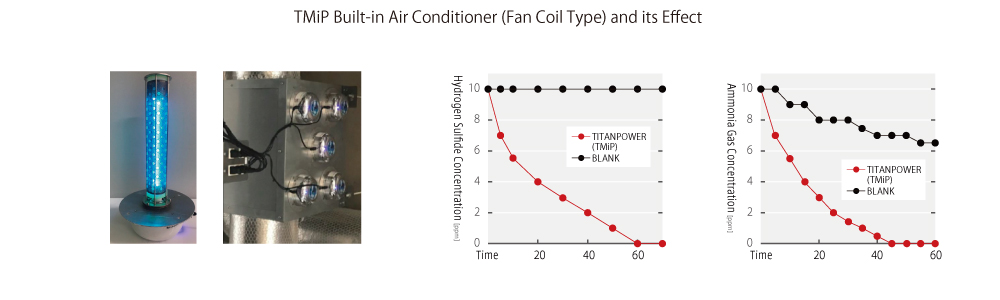
②TMiP (Titanium Mesh Impregnated Photocatalyst) is a mesh filter which is supported on anatase type titanium oxide plate specially processed with photocatalyst. Its light, soft and porous structure makes it easy to form various shapes. When combined with UV sterilization light, the sterilization and deodorization effects can be obtained.
【References】
*1 Guidelines for infection control in medical facilities, Ministry of Health, Labour and Welfare
https://www.mhlw.go.jp/bunya/kenkou/kekkaku-kansenshou04/pdf/08-06-04.pdf (May 19, 2020)
*2 Guide for dealing with novel coronavirus infections in healthcare institutions (ver.2.1), Japanese Society for Infection Prevention and Control
http://www.kankyokansen.org/uploads/uploads/files/jsipc/COVID-19_taioguide2.1.pdf (May 19, 2020)
*3 How to prevent the new coronavirus, Ministry of Health, Labour and Welfare
https://www.mhlw.go.jp/content/10900000/000599643.pdf (May 19, 2020)
*4 Guide to treatment of novel coronavirus infections (COVID-19) 1st edition, Ministry of Health, Labour and Welfare
https://www.mhlw.go.jp/content/000609467.pdf (May 19, 2020)
*5 Ventilation method to improve “closed space with poor ventilation”, Ministry of Health, Labour and Welfare
https://www.mhlw.go.jp/content/10900000/000618969.pdf (May 19, 2020)